Michigan doctor near death among first to get coronavirus plasma treatment
Donated plasma from the blood of recovered COVID-19 patients is showing early promise for treating those most sickened by the virus, Henry Ford Health System doctors said Tuesday.
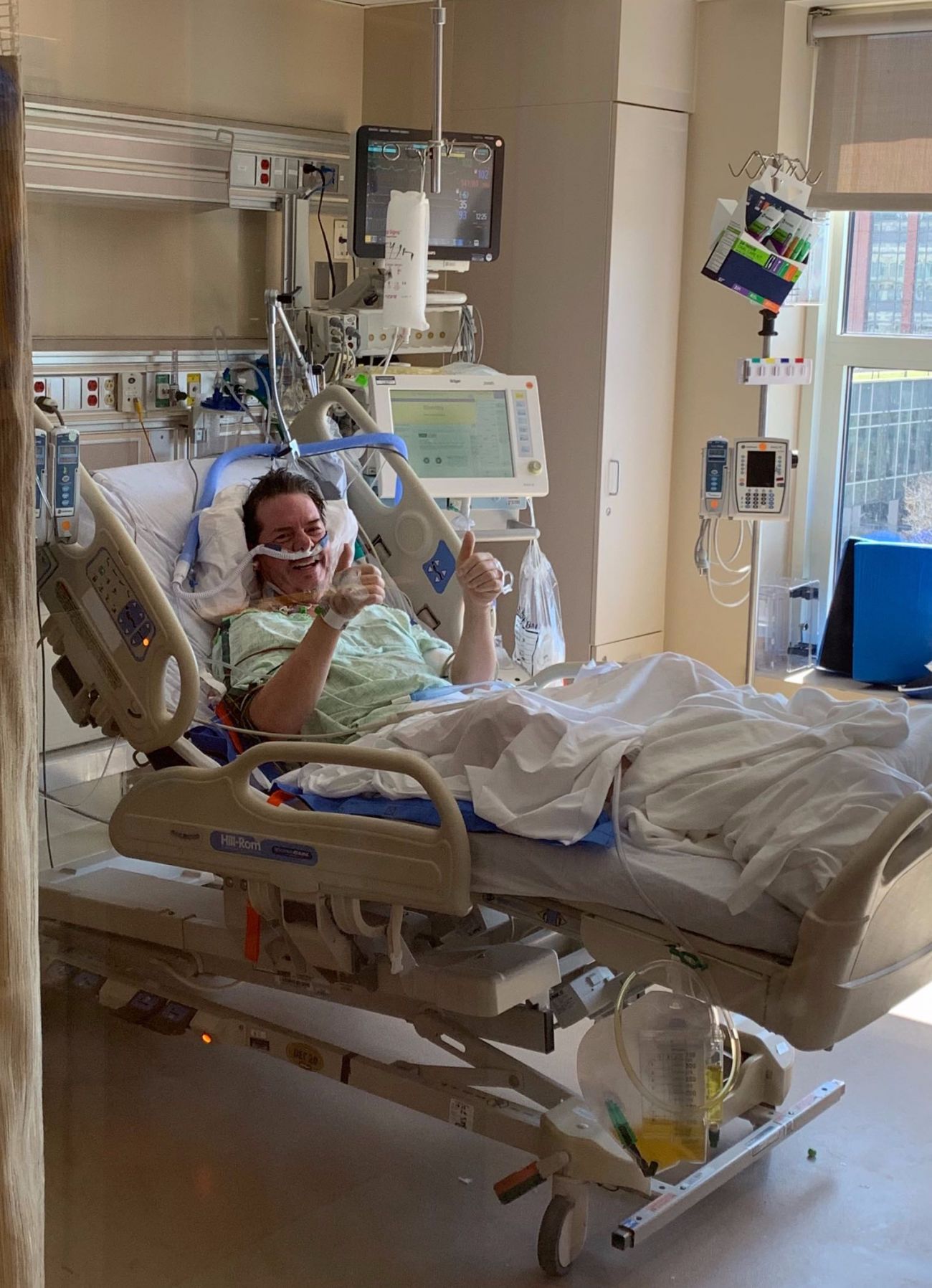
That includes Dr. Scott Kaatz, who worked on the front lines at Detroit’s Henry Ford Hospital as COVID-19 bore down on the city, then nearly died after being infected himself.
Kaatz, 62, a board-certified hospitalist, said Tuesday he was “unconscious, paralayzed, on a ventilator and face-down” at the hospital where he has worked for more than three decades. He’d already had a Skype phone call with his family they all thought might be their last.
Kaatz is among 14 patients treated experimentally with convalescent plasma at Henry Ford in recent weeks, the health system said.
“We've not had anybody with any complications and, in fact, many if not most of them ... have all made significant recoveries,” Dr. Steven Kalkanis, CEO of the Henry Ford Medical Group and the system’s chief academic officer, told reporters.
The plasma is being donated by people confirmed to have recovered from a COVID-19 infection who then have an immune response to the virus.
Doctors said the donated plasma may help others fighting a COVID-19 infection. Anecdotally at least, it seems promising, though it’s too early to know if the treatment actually works. Researchers hope it might even help those with underlying medical conditions or who are most highly exposed to the virus, such as health care workers and front-line responders, to ward off infection.
If a second wave of COVID-19 strikes, convalescent plasma might be a treatment option. Right now, there are several experimental options but no federally-approved drugs to treat COVID-19.
In fact, the Henry Ford patients were all given other experimental regimens, including the drugs hydroxychloroquine and Remdesivir, which have had mixed results treating COVID-19, and Interleukin 6, a drug that may help protect the lungs from the worst damage by the virus.
Only a large-scale analysis will reveal the effectiveness of convalescent plasma, Kalkanis noted. Indeed, it was just about a month ago that the U.S. Food and Drug Administration announced efforts to collect convalescent plasma to help fight this novel strain of the coronavirus.

Plasma testing begins around the country
The Henry Ford cases are among thousands across the country, said Dr. Nigel Paneth, a Michigan State University professor who’s helping lead efforts in the National COVID-19 Convalescent Plasma Project.
Paneth also spearheaded the group’s website, which will help distribute information on the Henry Ford cases and others to health care providers and plasma donors across the country.
The local efforts supplement a large-scale study, led by the Mayo Clinic, under which hundreds of people have received treatments, Paneth said. Ideally, researchers will be able to compare the results of the patients who received convalescent plasma against patients in the same hospitals that did not receive plasma to determine whether plasma played a role in recovery.
A half-dozen additional clinical trials are underway across the country into the use of convalescent plasma for COVID-19 patients, he said.
For now, doctors at least are filing anecdotal evidence of the plasma’s use through the website for its “rapid evaluation program” — a simple look at first results. So far, there have been no significant reports of complications, Paneth said.
“The early impressions look positive, but guardedly positive,” he said.
Researchers hope to have a better understanding within months, he said.
“If we don’t have a close to 80 to 90 percent answer in two or three months, I’d be disappointed.”
‘If I’m gone, what will they go through?’
During a press call Tuesday, Scott Kaatz and his wife, Meg, recalled how, as his condition worsened, a Skype call was arranged with his family.
Meg Kaatz, who has an underlying medical condition, had traveled to Texas in March to be with her son as the coronavirus struck Detroit.
Scott grew ill and, on April 4, he was admitted to his own hospital as a patient. His condition worsened. By mid-April, the news was grim: Doctors wanted to put him on a ventilator.
Options were running out. He wasn’t getting enough oxygen.
“I knew ... the signs were bad,” said Meg, a nurse.
Scott knew, too.
“My fear was for my family: If I’m gone, what will they go through,” said the doctor, a father of two and a grandfather.
On April 12, struggling for breath, Kaatz was unable to speak to his wife or adult children on the Skype call. He communicated with hand gestures and facial expressions.
“There were a lot of ‘I love yous,’ Meg Kaatz said.
Hours later, Scott was intubated and put on a ventilator.
Sometime after that, he fell unconscious and was started on the convalescent plasma treatment.
He awoke on April 18.
Kaatz said Tuesday that when he came to, he knew he was in a different room. There was sun from a window. He looked at his toes to make sure he wasn’t hallucinating.
He did not know he had received donated plasma days earlier. But he knew “that I survived.”
Fighting an invading enemy
When exposed to a virus or other disease, the body responds by producing antibodies within blood plasma to fight the virus and attempt to prevent it from spreading. In most cases, the antibodies remain for a time (convalesce) even after the infection is thwarted, standing guard to fight the virus again should it return.
In the past — think the Spanish flu of 1918, or more recently H1N1 or SARS — convalescent plasma from a surviving patient could be transfused into someone with the same virus to boost their immunities. Researchers are hoping history will repeat itself with COVID-19 but, again, since the virus is new, it’s too soon to tell.
Already, thousands of people with high antibodies have been identified through screening around the country, including in metro Detroit. Earlier this month, Beaumont Health’s Research Institute launched the nation’s largest serological testing study to help determine if COVID-19 antibodies offer protection after infection.
But on Tuesday, Scott Kaatz, healthy again, was able to focus on laughter with his wife during a virtual news conference — him, from his home study in Troy, and Meg from her son’s home in Texas.
“The kids told me that I had this really scruffy beard that I got for a couple of weeks,” Scott Kaatz said. “When I woke up I said ‘Hi honey, how are you doing?’ She said “With that beard, I don't know. Maybe we should have pulled the plug.’”
Kalkanis, also on the call, noted that his Henry Ford colleague “is looking healthy as ever from home” a little over a week after he nearly died.
He, too, was feeling hopeful.
“Now again, we don't have a scientific basis for evidence of a large scale trial yet. We're still analyzing the data,” Kalkanis said. “But all indices so far are very positive.”
See what new members are saying about why they donated to Bridge Michigan:
- “In order for this information to be accurate and unbiased it must be underwritten by its readers, not by special interests.” - Larry S.
- “Not many other media sources report on the topics Bridge does.” - Susan B.
- “Your journalism is outstanding and rare these days.” - Mark S.
If you want to ensure the future of nonpartisan, nonprofit Michigan journalism, please become a member today. You, too, will be asked why you donated and maybe we'll feature your quote next time!








