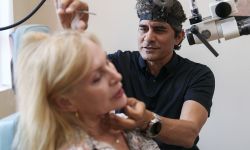
Which Michigan school COVID measures work? We asked scientists

Sept. 30: Michigan counties dump mask rules for thousands of pupils amid budget mess
Sept. 30: Science says school masks work. Public opinion is another issue in Michigan
Sept. 14: Republicans advance bills to bar Michigan school mask mandates
Sept. 8: Michigan: Masked or vaxxed students more likely to avoid COVID quarantine
In the Gibraltar School District in Wayne County, they’re taking down Plexiglas partitions. In Holt Public Schools in Ingham County, clear plastic shields are everywhere.
And in all Michigan districts, the recommended safe space between desks has been cut in half since last year — from 6 feet apart to 3 feet.
About 1.5 million students have already returned or are preparing to return to Michigan classrooms for the fall, and they may well see some different mitigation measures in their schools, as well as from district to district.
Related:
- Majority of Michigan students must now mask up, as Ingham, Washtenaw add rules
- More Michigan 3rd-graders struggled to read amid COVID, remote learning
- See how your Michigan school fared in the 2021 M-STEP test
- Michigan student test scores slump, as COVID halts slow progress
- Costs rising for Michigan COVID care with return of deductibles, copays
- After months of Michigan school mask protests, anti-anti-maskers mobilize
As their understanding of a still-new and shifting virus evolves, researchers, public health officers and school leaders have learned more about what measures help slow viral spread in schools, and what efforts employed last year didn’t provide much benefit.
For example, there’s broad acceptance among U.S. health institutions on the benefits of masking, with both the Centers for Disease Control and the American Academy of Pediatrics recommending universal masking in U.S. schools this fall (though that guidance has some medical critics, who say the evidence for requiring students to mask isn’t as strong).
There’s less enthusiasm for other measures schools employed last year, in those first, frightening, throw-the-kitchen-sink months of the pandemic, such as Plexiglas partitions and wholesale daily deep cleans of schools.
Studies conducted so far come with a myriad caveats — there are no “control groups” in a pandemic, and mitigation efforts are often used in combinations, making it difficult to distinguish the value of one measure versus another. Still, research of COVID-19 and efforts to slow its spread offer useful clues for Michigan schools.
Bridge Michigan examined dozens of studies and spoke with school officials, scientists and researchers about what has been found to work well, and what has less utility in keeping COVID-19 out of classrooms.
Here’s what we found:

Masks
During the pandemic last year, face masks were mandated for in-person classes. But children and their families face a mixed bag of mask policies as they return this fall, with a hodgepodge of local mask policies, and fiery debates about COVID protocols at school boards across Michigan.
As of Monday, more than half of the state’s public school students returning to class this fall are in counties or districts that have ordered some or all students to wear face coverings.
Some districts and county health departments are mandating masks only for elementary students — who are not yet eligible for vaccines, while others are requiring all staff and students, K-12, to wear masks regardless of vaccine status.
In Great Britain and some other European countries, students don’t wear masks, with schools instead trying to limit the spread of infection through quarantines and rapid testing. Earlier this month, the World Health Organization was more equivocal than the CDC on the issue, saying the “benefits of wearing masks in children for COVID-19 control should be weighed against potential harm associated with wearing masks, including feasibility and discomfort, as well as social and communication concerns.”
The WHO noted, however, that it isn’t saying masks don’t help limit spread of COVID, and studies on the impact of masks on COVID-19 spread indicate “mask wearing reduces transmissibility per contact.”
In the United States, the Centers for Disease Control and Prevention, the American Academy of Pediatrics and the American Medical Association strongly recommend student face masks, and a Duke University report noted that masks were effective in reducing the spread of COVID-19 in schools studied in North Carolina.
In Michigan, the administration of Gov. Gretchen Whitmer also recommends masks, though it has declined to impose mandates, leaving that decision (and the blowback from some parents that comes with it) to local officials.
There are some health experts who’ve raised questions about universal student masking, citing a CDC study involving students in Georgia, released in May. The study found requiring masks of teachers and staff had a significant impact in reducing COVID transmission, but that the 21 percent reduction found in the study in schools that “required mask use among students was not statistically significant (in reducing spread) compared with schools where mask use was optional.”
It’s important to note that the same CDC study still recommended universal mask wearing in schools, pointing to an October 2020 study that found masks have a “protective effect” in limiting the spread of the virus, particularly when masks are worn by those who are infected.
Health experts Bridge interviewed endorsed student mask requirements, saying they are one in a collection of preventive measures schools can leverage to limit infection and keep schools open this fall as children return to classrooms.
Masks are the “first layer of protection” against COVID, but “the battles over masking obscure the fact that masks are the base layer of a suite of tools,” said Alison Bernstein, an assistant professor of translational neuroscience at the Michigan State University College of Human Medicine and member of the group, SciMoms, a website which offers science-based information to parents.
She and other infectious disease experts say there’s no single way to stop COVID’s spread. Vaccines are effective but, as with other COVID safety protocols, are not 100 percent effective. Masks stop most particles, but not all.
The strategy, then, is to layer safety measures to limit the virus, one on top of the other, like piling slices of Swiss cheese to cover holes in other layers, said Dr. Matthew Sims, head of infectious diseases research at Beaumont Hospital in Royal Oak.
Dr. Teena Chopra, an infectious disease expert at Wayne State University, said masks also are crucial for children too young to be vaccinated. But, she noted, not all masks are created equal — and that children need to wear properly fitted masks.
Among the experts she turns to is Aaron Collins who goes by the name #masknerd on social media. Collins, whose background is in mechanical engineering and aerosol science, tests the filtration efficiency of hundreds of masks and keeps an open, searchable document of his results. In addition to filtration, Collins said parents must keep in mind fit and comfort to ensure children keep them on.
“The mask you don’t wear is one that doesn’t work,” he said in a recent message for parents.

Plexiglas
Acrylic dividers can help in certain situations. But they can make things worse, too.
It’s common sense that Plexiglas and similar shields separate you from the sneeze or cough blast in front of you that could contain the droplets that can carry the coronavirus, said Sims at Beaumont.
So the dividers can help in places such as salons and grocery stores, he said.
“Have you ever coughed or sneezed in the car, and you can’t take your hand off the wheel at that moment?” he said. “You know what your windshield looks like. Well, that’s what Plexiglas catches.”
But if they’re overused, those same barriers can also seal contaminants into a small space, Sims said.
In a classroom setting, a more effective deterrent to viral spread is improving ventilation, he and others said.
Gibraltar Superintendent Amy Conway said her district is removing acrylic partitions in classrooms this year. She said data from last school year showed little difference in COVID infection rates between districts like Gibraltar that installed clear shields, and nearby districts that did not. The study involving Georgia students also found desk barriers had little effect.
Gibraltar’s primary mitigation measures will be “masking and cleaning,” Conway said.
Kevin Van Den Wymelenberg, director of the Institute for Health in the Built Environment at the University of Oregon, told New York Magazine that Plexiglas would be useful in stopping large droplets “if students are close and coughing,” acting much like a sneeze guard at a salad bar. But if children already are wearing masks, “there is little effect from the barrier.”
Indeed, there is some evidence they can make classroom conditions worse, impeding the airflow of breath particles that a building ventilation system would otherwise flush out and replace with fresh air.
“Everybody’s aerosols are going to be trapped and stuck there and building up, and they will end up spreading beyond your own desk,” Linsey Marr, a professor of civil and environmental engineering at Virginia Tech and an authority on viral transmission, told The New York Times.
Ventilation upgrades
Many schools have made improvements to ventilation systems or are planning to use COVID school relief funds to renovate sometimes decades-old heating, ventilation and air conditioning.
That’s important because small particles can stay in the air for hours or days; good ventilation can help reduce the proportion of airborne contaminants.
The Georgia study found coronavirus infections were 39 percent lower in schools that had improved ventilation systems than in schools that had not.
Even without expensive HVAC improvements, teachers can improve ventilation through “dilution” efforts — opening doors and windows or using portable air purifiers and fans to dilute air contaminants in the air, experts said. Fans, for instance, should be used to move potentially contaminated air outdoors, rather than simply circulating it in small spaces.
“Don’t forget to open windows on school buses,” Emily Somers, an associate professor and epidemiologist at the University of Michigan, wrote to Bridge in an email.
Educators also can construct affordable, do-it-yourself versions of purifiers that some testing has shown work with surprising efficiently. They’re called Corsi-Rosenthal Boxes, Somers said, and require little more than a box fan, MERV 13 filters, and some time.
Schools should also consider shifting activities outdoors when feasible, especially activities in which higher levels of airborne viruses are expected to accumulate and spread, such as lunch, choir and band, Somers said.
In a February review in the Journal of Infectious Diseases, authors found that the odds of indoor transmission are 18.7 times higher than outdoor transmission.
Social distancing
Last school year, state health officials recommended that Michigan schools that held in-person instruction should keep desks 6 feet apart to try to decrease COVID spread. That policy that made it nearly impossible for schools to have all students in classrooms at the same time.
But in a study published in March, researchers who reviewed infection rates in 251 Massachusetts school districts with more than a half-million students found no significant difference in spread between districts that adopted 6-feet versus 3-feet social distancing.
The CDC updated its recommendations to reflect the change, but even that is layered with variables, said Dr. Peter Gulick, an infectious disease expert at Michigan State University.
A reduction in social distancing can be problematic in poorly ventilated areas or when vaccination rates are low, for example, he said. In those cases, weekly testing is advised.
Surface sanitization
Some schools last year invested in high-tech cleaning machinery and wipes, spray bottles and hand sanitizers became a constant companion for teachers — efforts developed at a time when scientists were still trying to understand precisely how COVID spreads.
Early studies found coronavirus could live on surfaces for days, but it became clear over time that the risk of its spread that way “is generally considered to be low,” according to the CDC.
That’s because the virus generally adheres to nasal passages, and isn’t adept at sticking to skin or making its way into nicks or scratches like a bacteria does, said Gulick at Michigan State.
Still, daily disinfecting is always a good idea, he argued, because it protects against other dangerous microorganisms such as Staphylococcus aureus, a common bacteria that can cause skin infections but also can enter the body and damage internal organs.
School officials who spoke to Bridge said they do not plan to cut back on ramped-up cleaning practices launched last year, and that’s still not a bad idea, said MSU’s Gulick.
Daily cleaning and disinfecting should be stepped up more frequently in areas where someone has coughed, and any area used by a sick person suspected of being infected.
Sanitizer
Alcohol-based hand sanitizers work against coronaviruses that cause the common cold, so it’s believed that it works against the coronavirus that causes COVID, too.
Sanitizers should have at least 60 percent alcohol or more, said Jamie Alan, an associate professor at the Michigan State University Department of Pharmacology and Toxicology.
The U.S. Food and Drug Administration, which has issued more detailed guidance here, also provides a list of hand sanitizer products to avoid.
And while sanitizer is believed effective against COVID-19, thoroughly washing hands with soap and water is best, experts say.
Temperature checks
Some schools checked the temperature of students, staff and visitors as they entered school buildings in the 2020-21 school year. The temperature checks were never mandated by the state, but they were included in the state’s return to school roadmap as a possible additional mitigation measure.
It’s unclear whether any school districts are continuing temperature checks this year.
Gulick at Michigan State questions the return on time invested in this measure.
Temperature checks aren’t going to flag students or staff who carry the virus but are asymptomatic, and he worried about temperature devices that aren’t working properly or people who aren’t properly working them.
In the setting of airports, another CDC study found that screening protocols that included temperature checks and symptom screening for passengers yielded few COVID cases, took up considerable resources and was unlikely to detect a majority of infected travelers.
See what new members are saying about why they donated to Bridge Michigan:
- “In order for this information to be accurate and unbiased it must be underwritten by its readers, not by special interests.” - Larry S.
- “Not many other media sources report on the topics Bridge does.” - Susan B.
- “Your journalism is outstanding and rare these days.” - Mark S.
If you want to ensure the future of nonpartisan, nonprofit Michigan journalism, please become a member today. You, too, will be asked why you donated and maybe we'll feature your quote next time!